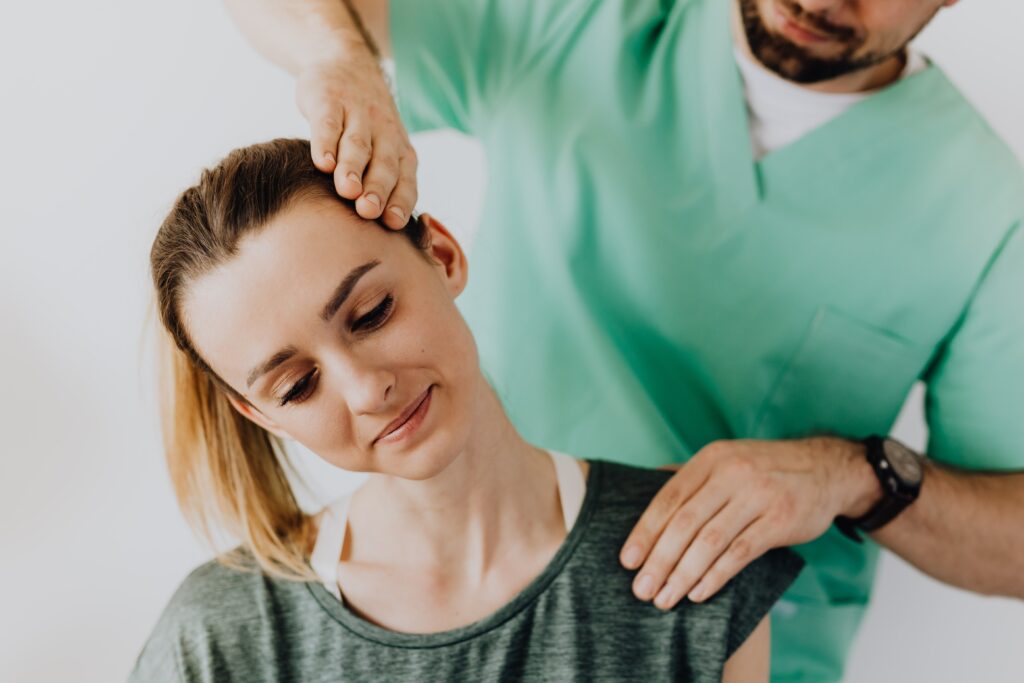
Effective Physical Therapy for Neck Facet Joint Dysfunction: Relieve Pain and Regain Mobility
Introduction
Neck facet joint dysfunction is a prevalent condition that causes inflammation and misalignment of the vertebrae in the cervical (neck) region, leading to pain and movement restrictions. The pain can be chronic, and the condition may keep worsening if left untreated. Unfortunately, many individuals with this condition do not seek medical attention until their symptoms become unbearable, leading to reduced quality of life.
Physical therapy has been shown to be an effective treatment option for neck facet joint dysfunction. It focuses on improving strength, flexibility, and range of motion, and reducing pain through manual therapy, exercises, and other techniques. It can restore function, mobility, and quality of life, helping individuals get back to their daily activities and improving their overall well-being. If you suffer from neck facet joint dysfunction, don’t wait until it becomes unbearable to seek medical attention. Talk to your doctor or physical therapist to explore treatment options that can help you manage your condition and improve your quality of life.
What to Expect at Physical Therapy
Physical therapy usually begins with a thorough assessment by a trained therapist who will evaluate your posture, muscle strength, and range of motion. The therapist may also use manual techniques such as massage, stretching, or joint mobilization to improve flexibility and reduce pain in certain areas. After completing the evaluation, your physical therapist will create an individualized treatment plan based on your goals and needs. This plan will likely include exercises targeting specific muscle groups that support your neck and upper back; strengthening these areas help decrease stress on the joints affected by neck facet joint dysfunction.
What Types Of Exercises Might You Do?
Your physical therapist may recommend any number of exercises depending on your particular diagnosis; however here are some common ones that target the muscles supporting your head and spine:
- Neck stretches: These stretches are designed to increase flexibility in tight areas while increasing circulation around painful areas
- Isometric exercises: These exercises involve contracting muscles without moving them against resistance such as weights or bands
- Range Of Motion Exercises: These exercises help you increase mobility in all directions while also improving coordination
- Core strengthening: Strengthening core muscles helps provide stability for your spine which can reduce strain on joints affected by neck facet joint dysfunction
How Long Does Recovery Take?
The length of time it takes to recover from neck facet joint dysfunction varies from person to person depending on severity and other factors. Generally speaking most people experience significant improvement within 4-6 weeks when participating in regular physical therapy sessions combined with home exercise programs tailored specifically for them by their physical therapist. With dedication and consistency, many find that they are able to return to their normal activities after several months of physical therapy.
Conclusion
Physical therapy can reduce pain and improve mobility in neck facet joint dysfunction. Targeting supporting muscle groups along with a range of motion exercises can improve posture and reduce stress. Commitment and consistency can lead to significant relief in 4-6 weeks and a return to activities after several months of therapy.
Research
Abdel-Aziem AA, Mohamed RR, Draz AH, Azab AR, Hegazy FA, Diab RH. The effect of McKenzie protocol vs. deep neck flexor and scapulothoracic exercises in subjects with chronic neck pain – a randomized controlled study. Eur Rev Med Pharmacol Sci. 2022;26(9):3138-3150. doi:10.26355/eurrev_202205_28731